Η PSORIATIC ARTHRITIS
Arthritis occurs in about 10% of patients with psoriasis. Psoriatic arthritis typically
develops after, or coincident with, the onset of psoriasis, but the arthritis precedes
the skin disease by as much as 2 years in a minority of cases (~15%). A range of
joint manifestations occurs in association with psoriasis: monarticular or oligoarticular
arthritis, polyarthritis, arthritis mutilans, and arthritis of the axial skeleton.
Two-thirds of patients with psoriatic arthritis have an asymmetric oligoarthritis
or a monoarthritis, but others have polyarticular disease that mimics osteoarthritis
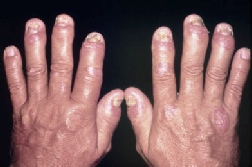
or rheumatoid arthritis in its distribution. Involvement of the distal interphalangeal
joints, which are spared by rheumatoid arthritis, can help distinguish psoriatic
arthritis from rheumatoid arthritis. Psoriatic arthritis of the distal interphalangeal
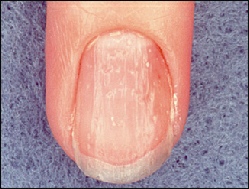
joints is associated with abnormalities of the nail bed and dystrophic changes of
the nail, such as pitting, onycholysis, ridging, and brown-yellow discoloration (oil-drop
sign).
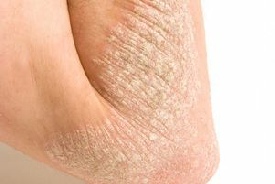
The skin disease can be subtle. When psoriatic arthritis is suspected based on the
distribution of affected joints or suspicious radiographic findings, skin examination
should include evaluation of the gluteal fold, umbilical region, and scalp because
cutaneous findings can be limited to these sites. Of significance, the explosive
development of psoriatic skin disease, with or without articular involvement, can
be a sign of HIV infection and should prompt appropriate testing
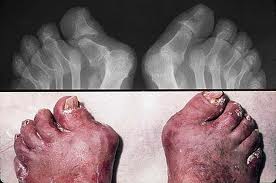
Psoriatic arthritis has a distinctive radiographic appearance, specifically the concurrence
of both bony destruction and proliferation at an affected site . In addition, psoriatic
arthritis can be highly destructive, with development of a pencil-in-cup appearance
of the finger bones, and in some cases, arthritis mutilans. Involvement of the axial
skeleton resembles that of reactive arthritis. Sacroiliitis is usually unilateral,
and nonmarginal syndesmophytes characterize the spondylitis.
THERAPY
NSAIDs are used for mild disease. Once-weekly methotrexate is effective for treatment
of both the cutaneous and peripheral articular disease. Sulfasalazine is superior
to placebo in the treatment of joint disease, but the effect, although statistically
significant, is small. Anti-TNF therapies show considerable promise and improve both
the articular and cutaneous manifestations of psoriatic arthritis. Cyclosporine A
has been used with severe, refractory disease.
Oral glucocorticoids should be avoided, but intra-articular injections of glucocorticoids
can be useful adjunctive therapy. Care should be taken to make certain that the needle
does not pass through psoriatic plaques, which are heavily contaminated with bacteria.
Psoriatic skin lesions overlying a joint are a contraindication to arthrocentesis
because of the added risk of procedure-induced septic arthritis.
 πίσω
πίσω