 πίσω
πίσω
COPYRIGHT © by Michaelidou Maria
Dr. Maria Michailidou
RHEUMATOID ARTHRITIS
General Considerations
Rheumatoid arthritis is a chronic systemic inflammatory disease whose major manifestation
is synovitis of multiple joints. It has a prevalence of 1% and is more common in
women than men (female:male ratio of 3:1). Rheumatoid arthritis can begin at any
age, but the peak onset is in the fourth or fifth decade for women and the sixth
to eighth decades for men. The cause is not known. Susceptibility to rheumatoid arthritis
is genetically determined with multiple genes contributing. Inheritance of class
II HLA molecules with a distinctive five-
The pathologic findings in the joint include chronic synovitis with formation of a pannus, which erodes cartilage, bone, ligaments, and tendons. In the acute phase, effusion and other manifestations of inflammation are common. In the late stage, organization may result in fibrous ankylosis; true bony ankylosis is rare. In both acute and chronic phases, inflammation of soft tissues around the joints may be prominent and is a significant factor in joint damage.
Clinical Findings in rheumatoid arthritis
Symptoms and Signs
Joint symptoms
The clinical manifestations of rheumatoid disease are highly variable, but joint symptoms usually predominate. Although acute presentations may occur, the onset of articular signs of inflammation is usually insidious, with prodromal symptoms of vague periarticular pain or stiffness. Symmetric swelling of multiple joints with tenderness and pain is characteristic. Monarticular disease is occasionally seen initially. Stiffness persisting for more than 30 minutes (and usually many hours) is prominent in the morning; the duration of morning stiffness is a useful indicator of disease activity. Stiffness may recur after daytime inactivity and be much more severe after strenuous activity. Although any diarthrodial joint may be affected, PIP joints of the fingers, MCP joints, wrists, knees, ankles, and MTP joints are most often involved. Synovial cysts and rupture of tendons may occur. Entrapment syndromes are not unusual—particularly of the median nerve at the carpal tunnel of the wrist. Rheumatoid arthritis can affect the neck but spares the other components of the spine and does not involve the sacroiliac joints.
Rheumatoid nodules
Twenty percent of patients have subcutaneous rheumatoid nodules, most commonly situated
over bony prominences but also observed in the bursae and tendon sheaths. Nodules
are occasionally seen in the lungs, the sclerae, and other tissues. Nodules correlate
with the presence of rheumatoid factor in serum ("seropositivity"), as do most other
extra-
Ocular symptoms
Dryness of the eyes, mouth, and other mucous membranes is found especially in advanced disease (see Sjögren's syndrome). Other ocular manifestations include episcleritis, scleritis, and scleromalacia due to scleral nodules
.
Basic Program (Nonpharmacologic Management)
The primary objectives in treating rheumatoid arthritis are reduction of inflammation
and pain, preservation of function, and prevention of deformity. Success requires
early, effective pharmacologic intervention and ongoing input by physical and occupational
therapists. Disease-
Education and emotional factors
The clinician should explain the disease, describe its fluctuations, and involve the patient and family in decisions about therapy.
Physical and occupational therapies
Physical and occupational therapists understand nonpharmacologic treatments of arthritis (described below) and can effectively teach them. The therapist can develop a program the patient can follow at home, with only periodic monitoring.
Systemic rest
The amount of systemic rest required depends on the presence and severity of inflammation.
With mild inflammation, 2 hours of rest each day may suffice. In general, rest should
be continued until significant improvement is sustained for at least 2 weeks; thereafter,
the program may be liberalized. However, the increase of physical activity must proceed
gradually and with appropriate support for any involved weight-
Articular rest
Decrease of articular inflammation may be expedited by joint rest. Relaxation and
stretching of the hip and knee muscles, to prevent flexion contractures, can be accomplished
by having the patient lie in the prone position for 15 minutes several times daily.
Sitting in a flexed position for prolonged periods is a poor form of joint rest.
Appropriate adjustable supports provide rest for inflamed weight-
Exercise
Exercises are designed to preserve joint motion, muscular strength, and endurance. Initially, for inflammatory disease, passive range of motion and isometric exercises (such as straight leg raising) are best tolerated. In hydrotherapy, the buoyancy of water permits maximum isotonic and isometric exercise with no more stress on joints than active range of motion exercises. As tolerance for exercise increases and the activity of the disease subsides, progressive resistance exercises may be introduced. Patients should follow the general rule of eliminating any exercise that produces increased pain 1 hour after the exercise has ended.
Heat and cold
These are used primarily for their muscle-
Assistive devices
Patients with significant hip or knee arthritis may benefit from having an elevated toilet, a gripping bar, or a cane. Patients hold the cane in the hand opposite to the affected knee or hip, thus leaning away from the affected joint. Crutches or walkers may be needed for patients with more extensive disease.
Splints
Splints may provide joint rest, reduce pain, and prevent contracture, but their use should be guided by certain principles.
a. Night splints of the hands or wrists (or both) should maintain the extremity in the position of optimum function. The elbow and shoulder lose motion so rapidly that other local measures and corticosteroid injections are usually preferable to splints.
b. The best "splint" for the hip is prone-
c. Splints should be applied for the shortest period needed, should be made of lightweight
materials for comfort, and should be easily removable for range-
d. Corrective splints, such as those for overcoming knee flexion contractures, should be used under the guidance of a clinician familiar with their proper use.
Note: Avoidance of prolonged sitting or knee pillows may decrease the need for splints.
Weight loss
For overweight patients, achieving ideal body weight will reduce the wear and tear placed on arthritic joints of the lower extremities.
Nonsteroidal Anti-
NSAIDs provide some symptomatic relief in rheumatoid arthritis but do not prevent erosions or alter disease progression. They are not appropriate for monotherapy and should only be used in conjunction with DMARDs. A large number of NSAIDs are available; all appear equivalent in terms of efficacy (see Table 5–3).
NSAIDs work in arthritis by the same mechanism that causes side effects: inhibition
of COX, the enzyme that converts arachidonic acid to prostaglandins. Although prostaglandins
play important roles in promoting inflammation and pain, they also help maintain
homeostasis in several organs—especially the stomach, where prostaglandin E serves
as a local hormone responsible for gastric mucosal cytoprotection. The discovery
that COX exists in two isomers—COX-
Celecoxib, a selective COX-
Corticosteroids
Low-
Methotrexate
Methotrexate is usually the initial synthetic DMARD of choice for patients with rheumatoid arthritis. It is generally well tolerated and often produces a beneficial effect in 2–6 weeks
Other symptoms
Palmar erythema is common. Occasionally, a small vessel vasculitis develops and manifests
as tiny hemorrhagic infarcts in the nail folds or finger pulps. Although necrotizing
arteritis is well reported, it is rare. Pericarditis and pleural disease, when present,
are usually silent clinically. Additional extra-
Aortitis is a rare late complication that can result in aortic regurgitation or rupture and is usually associated with evidence of rheumatoid vasculitis elsewhere in the body.
Laboratory Findings
Anti-
The ESR and levels of C-
Imaging
Of all the laboratory tests, radiographic changes are the most specific for rheumatoid
arthritis. Radiographs obtained during the first 6 months of symptoms, however, are
usually normal. The earliest changes occur in the wrists or feet and consist of soft
tissue swelling and juxta-




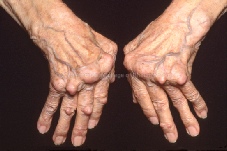
Photos of rheumatoid arthritis